Binge Eating and Hormonal Regulation: Emotional Hunger
Our entire evolution, we were like any other species on this planet, in constant hunger and in search of food. Overeating is an example of maladaptation.
Milos Pokimica
Written By: Milos Pokimica
Medically Reviewed by: Dr. Xiùying Wáng, M.D.
Updated June 9, 2023For our entire evolution, we were like any other species on this planet in constant search of food. We were not obese but in a state of constant hunger and constant physical activity. This was the case for all of our ancestor species and that means the time period of 50 million years.
Technological progress that happened in the last couple of hundreds of years didn’t change our body physiology. It is an abrupt shift in evolutional terms. The feeling of constant fullness, on the other hand, is not natural, and it is an example of maladaptation. Our hominin ancestors and even homo sapiens dint have technology and food on every corner. Hunger is a normal feeling and it is a normal feeling for every animal. Because of our evolutionary conditioning and the way our brain works, people even if we are on a restrictive diet cannot deal with the feeling of constant hunger. We want to have a feeling of fullness and there is nothing we can do about it. So here comes caffeine, hunger suppressors of different kinds and medicine and surgeries, and so on.
In an evolutionary sense, this is protective behavior, because there is an extreme scarcity of food, bingeing as much as we possibly can is a good survival strategy. But what happens when we have an overabundance of food and we never had that abundance during our entire existence including our direct ancestor species. Our evolution didn’t begin with the modern human species we have just become a little smarter. Most of our genes and the body are the same, especially in basic survival mechanisms that didn’t have to change for millions of years.
All of this would not have to be an issue but obesity is everything but a cosmetic issue. Most people do understand this but are unable to do anything about it because of fear of starvation. This fear is instinctive and it would override any logical behavior and in reality, we would always overeat. Weight gain comes slowly and in a prolonged period. Even if we gain just a little on a monthly basis, in time this little would be too much.
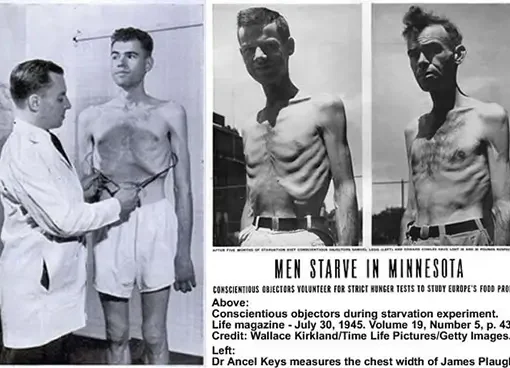
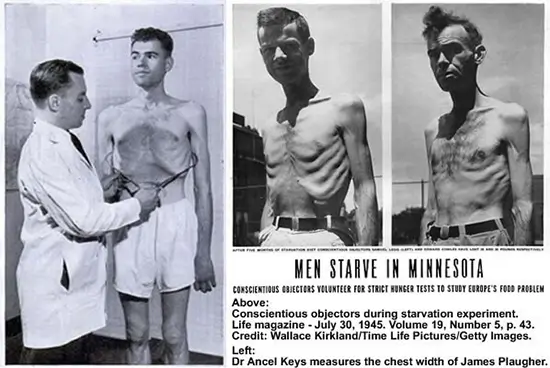
When an individual starts to have a restrictive diet the instinctive fear of starvation will have an impact on behavior and more than just in the psychological way. It will trigger different pathways in the brain that are responsible for appetite control, fear, reward mechanism (how much pleasure we get from pleasurable experiences), and most of our brain functioning. And this will not stop when we go off the diet but will continue as a never-ending story. It is a so-called “yo-yo” effect. Even since a Minnesota starvation experiment (Kelesidis et al., 2010) scientists have been aware of the full scope of effects that a restrictive diet can have on someone’s behavior.
The way that the brain works is by the “carrot and a stick” mechanism. Number one would be the avoidance of pain, and when pain is avoided pleasure-seeking comes into play.
The more pain the stronger behavioral changes. The problem is until the pain is removed the pleasure-seeking does not exist. For example, people in the Minnesota starvation experiment after a period of time couldn’t think of anything else except food. They could not take the pain of constant hunger. After they were given food the fear of starvation never went away and they were overeating and binging as much as they could and have become obese in a very short period. But this behavior exists just to a smaller extent in everyday “normal” behavior. The most normal feeling of hunger had become much more pronounced because today we cannot deal with hunger because we have never experienced the real level of starvation. That is the reason why most of us cannot really cope well with dieting because we do not have tolerance for pain anymore. And even if we do, the normal response of the brain will be to go into survival avoidance of pain mode and cut off all pleasure-seeking behavior until the hunger is removed. It is not possible to be in a state of hunger and enjoy life. Especially because now we are removed from our natural environment and we have supernormal stimuli everywhere. Even a normal feeling of hunger is something that we cannot take as a normal feeling anymore.
Our behavior has been conditioned in such a way that our brain has down-regulated its pleasure response. For example, this happens to heroin addicts. Heroin is one of the strongest drugs in existence. It gives a lot of pleasure. But in time addicts will become more tolerant of the effects of it to some extent because their brain adapts. The same thing has happened in our modern society. Our brain has to some extent adapted to supernormal stimuli from food and hunger has become a much more pronounced feeling than it would be in normal animal species. Because of lack of scarcity food is not as a big reward as it used to be especially because of unnaturally high concentrations and combinations of energy sources that do not exist in nature.
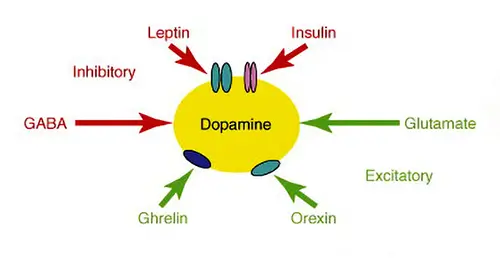
Extracted sugar and extracted fat do not exist in nature and it is digested much quicker than in normal circumstances from whole food sources giving us a dopamine high. Especially the combination of sugar and fat (Zhang et al., 2005). This combination does not exist in nature. Because of this dieting has become a form of addiction much more than it would be in a natural environment.
The result of this is that we have become obese and there is nothing we can do about it. Today nearly 70% of American adults are either overweight or obese.
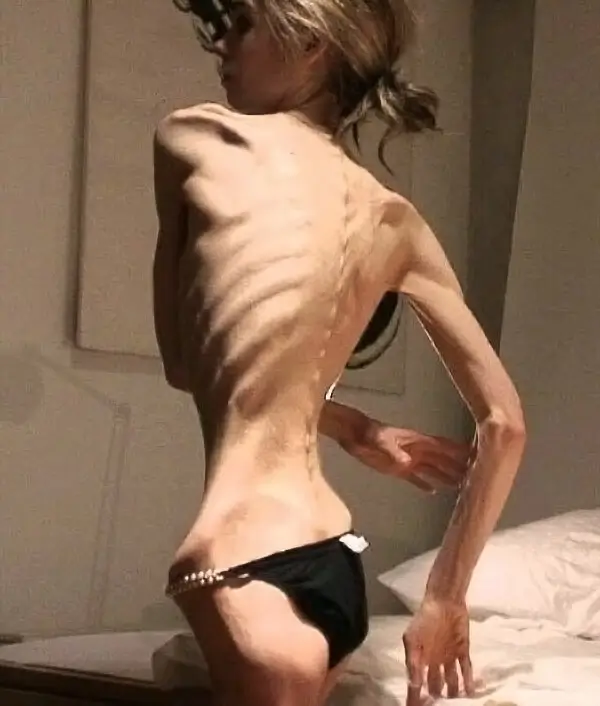
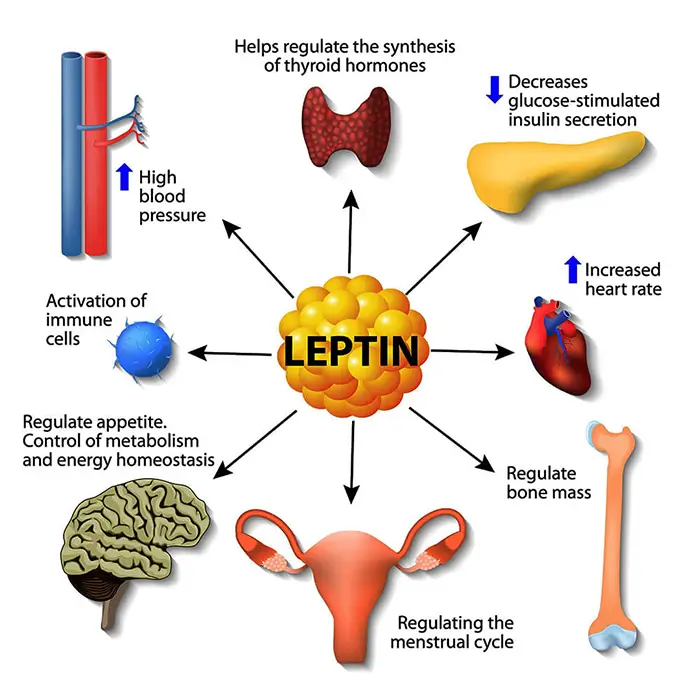
Actually, even anorexia nervosa patients are victims of the same maladaptation. It is not a psychological issue it is conditioned behavior of pleasure and pain reward mechanisms. In anorexia patients, there is also malfunction but in the opposite direction. When they refeed themselves, their plasma leptin concentration will increase rapidly and reach roughly normal levels long before normal weight is achieved (Obradovic et al., 2021). Thus keeping them anorexic. They experience hunger much less than someone that does not have this condition. Excessive leptin production and its effect on the feeling of fullness could play a permissive role in the pathogenesis of this condition.
Leptin is the satiety hormone, and it is opposed by the actions of another hormone named ghrelin, the hunger hormone. Both hormones act on the receptors in the brain to regulate appetite (Zhang et al., 2017). When people think that their conscious mind will have an impact on their behavior I always asked them to do an experiment and try to keep their breath. After a minute or so there will be pain singling and the unconscious part of the brain will override our behavior. The signal is due to the fact that the brain is dying and no matter what, you have to take oxygen in or die. We will gasp for breath no matter how strongly we resist. This is a reason that someone can drown in 20 seconds if panic kicks in. The same behavior changes affect our day-to-day behavior in regard to the water we drink, the air we breathe and the food we eat.
The balance of these two hormones is necessary to achieve an overall energy balance in the body. In obesity, a decreased sensitivity to leptin occurs (Anderberg et al., 2016). This is a big problem that will result in a brain’s inability to detect satiety despite high energy stores in the rest of the body. Why does this happen? The basis for leptin resistance in obese human subjects is unknown. If leptin levels remain persistently raised due to overeating, there may be a downregulation of the leptin receptors and hence decreased sensitivity to the hormone. In humans, and actually in any other animal low leptin levels induced by a low-calorie diet resulted in a decrease in plasma leptin concentration triggering high levels of constant hunger. This may explain the high failure rate of dieting. Low leptin levels are likely to be a powerful stimulus to weight gain.
In the case of obesity, the standard regulatory system will tell the brain that we have fat deposits stored for an extended period and that we can endure little hunger. The problem is that we could never become fat due to scarcity, so we never developed an adaptation to the abundance of food. Our mind still thinks that if we do not eat all that we can we will starve to death in the upcoming drought.
References:
- Kelesidis, T., Kelesidis, I., Chou, S., & Mantzoros, C. S. (2010). Narrative review: the role of leptin in human physiology: emerging clinical applications. Annals of internal medicine, 152(2), 93–100. https://doi.org/10.7326/0003-4819-152-2-201001190-00008
- Zhang, F., Chen, Y., Heiman, M., & Dimarchi, R. (2005). Leptin: structure, function and biology. Vitamins and hormones, 71, 345–372. https://doi.org/10.1016/S0083-6729(05)71012-8
- Obradovic, M., Sudar-Milovanovic, E., Soskic, S., Essack, M., Arya, S., Stewart, A. J., Gojobori, T., & Isenovic, E. R. (2021). Leptin and Obesity: Role and Clinical Implication. Frontiers in endocrinology, 12, 585887. https://doi.org/10.3389/fendo.2021.585887
- Zhang, Y., & Chua, S., Jr (2017). Leptin Function and Regulation. Comprehensive Physiology, 8(1), 351–369. https://doi.org/10.1002/cphy.c160041
- Anderberg, R. H., Hansson, C., Fenander, M., Richard, J. E., Dickson, S. L., Nissbrandt, H., Bergquist, F., & Skibicka, K. P. (2016). The Stomach-Derived Hormone Ghrelin Increases Impulsive Behavior. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology, 41(5), 1199–1209. https://doi.org/10.1038/npp.2015.297
- Kalm, L. M., & Semba, R. D. (2005). They starved so that others be better fed: remembering Ancel Keys and the Minnesota experiment. The Journal of nutrition, 135(6), 1347–1352. https://doi.org/10.1093/jn/135.6.1347
- Tobey J. A. (1951). The Biology of Human Starvation. American Journal of Public Health and the Nations Health, 41(2), 236–237.[PubMed]
- Howick, K., Griffin, B. T., Cryan, J. F., & Schellekens, H. (2017). From Belly to Brain: Targeting the Ghrelin Receptor in Appetite and Food Intake Regulation. International journal of molecular sciences, 18(2), 273. https://doi.org/10.3390/ijms18020273
- Müller, M. J., Enderle, J., Pourhassan, M., Braun, W., Eggeling, B., Lagerpusch, M., Glüer, C. C., Kehayias, J. J., Kiosz, D., & Bosy-Westphal, A. (2015). Metabolic adaptation to caloric restriction and subsequent refeeding: the Minnesota Starvation Experiment revisited. The American journal of clinical nutrition, 102(4), 807–819. https://doi.org/10.3945/ajcn.115.109173
- Dulloo A. G. (2021). Physiology of weight regain: Lessons from the classic Minnesota Starvation Experiment on human body composition regulation. Obesity reviews : an official journal of the International Association for the Study of Obesity, 22 Suppl 2, e13189. https://doi.org/10.1111/obr.13189
- LASKER G. W. (1947). The effects of partial starvation on somatotype: an analysis of material from the Minnesota starving experiment. American journal of physical anthropology, 5(3), 323–341. https://doi.org/10.1002/ajpa.1330050305
- Dulloo, A. G., Jacquet, J., & Girardier, L. (1996). Autoregulation of body composition during weight recovery in human: the Minnesota Experiment revisited. International journal of obesity and related metabolic disorders : journal of the International Association for the Study of Obesity, 20(5), 393–405.[PubMed]
- Keys et al. (1950) “The Biology of Human Starvation (2 volumes)”. University of Minnesota Press.
Related Posts
Sources:
Do you have any questions about nutrition and health?
I would love to hear from you and answer them in my next post. I appreciate your input and opinion and I look forward to hearing from you soon. I also invite you to follow us on Facebook, Instagram, and Pinterest for more diet, nutrition, and health content. You can leave a comment there and connect with other health enthusiasts, share your tips and experiences, and get support and encouragement from our team and community.
I hope that this post was informative and enjoyable for you and that you are prepared to apply the insights you learned. If you found this post helpful, please share it with your friends and family who might also benefit from it. You never know who might need some guidance and support on their health journey.
– You Might Also Like –

Learn About Nutrition
Milos Pokimica is a doctor of natural medicine, clinical nutritionist, medical health and nutrition writer, and nutritional science advisor. Author of the book series Go Vegan? Review of Science, he also operates the natural health website GoVeganWay.com
Medical Disclaimer
GoVeganWay.com brings you reviews of the latest nutrition and health-related research. The information provided represents the personal opinion of the author and is not intended nor implied to be a substitute for professional medical advice, diagnosis, or treatment. The information provided is for informational purposes only and is not intended to serve as a substitute for the consultation, diagnosis, and/or medical treatment of a qualified physician or healthcare provider.NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY SEEKING MEDICAL TREATMENT BECAUSE OF SOMETHING YOU HAVE READ ON OR ACCESSED THROUGH GoVeganWay.com
NEVER APPLY ANY LIFESTYLE CHANGES OR ANY CHANGES AT ALL AS A CONSEQUENCE OF SOMETHING YOU HAVE READ IN GoVeganWay.com BEFORE CONSULTING LICENCED MEDICAL PRACTITIONER.
In the event of a medical emergency, call a doctor or 911 immediately. GoVeganWay.com does not recommend or endorse any specific groups, organizations, tests, physicians, products, procedures, opinions, or other information that may be mentioned inside.
Editor Picks –
Milos Pokimica is a health and nutrition writer and nutritional science advisor. Author of the book series Go Vegan? Review of Science, he also operates the natural health website GoVeganWay.com
Latest Articles –
Top Health News — ScienceDaily
- Scientists reversed biological age in older adults with a 4-week diet changeon May 12, 2026
A four-week diet change was enough to make some older adults appear biologically younger in a new University of Sydney study. Participants who reduced fat intake or shifted toward more plant-based protein showed improvements in key health biomarkers tied to aging. The strongest results came from a lower-fat, higher-carb diet, while people eating closer to their usual diets saw almost no change.
- Scientists discover hidden fat-burning switch that could strengthen boneson May 12, 2026
Scientists at McGill University have uncovered a hidden molecular “switch” that turns on a powerful calorie-burning system in brown fat — the body’s heat-generating fat linked to metabolism and weight control. The breakthrough centers on glycerol, a molecule released when fat is broken down in the cold, which activates an enzyme called TNAP and triggers an alternative heat-producing pathway that scientists had struggled to explain for years.
- This simple strength test could predict how long you liveon May 12, 2026
Staying strong may be one of the biggest secrets to living longer — especially for older women. A major study of more than 5,000 women found that simple signs of muscle strength, like a firm hand grip or the ability to quickly stand up from a chair, were strongly linked to lower risk of death over the next eight years.
- Scientists say this common sweetener may be quietly rewiring your metabolismon May 11, 2026
Researchers say fructose is not just “empty calories” — it may actively push the body toward fat storage and metabolic disease. A new review found that fructose affects the body differently from glucose, disrupting normal energy regulation and promoting processes linked to obesity, insulin resistance, and cardiovascular problems.
- Ozempic delivers major weight loss in adults over 65, study findson May 11, 2026
A major new analysis suggests semaglutide (Ozempic, Wegovy) works remarkably well in adults over 65, helping many lose substantial amounts of weight while improving heart and metabolic health. Participants taking the drug lost over 15% of their body weight on average — far more than those receiving placebo treatment. Many also moved out of obesity categories entirely and reached healthier weight levels.
- Researchers say AI chatbots may blur the line between reality and delusionon May 11, 2026
A new study suggests AI chatbots may do more than spread misinformation — they can actively strengthen a user’s false beliefs. Because conversational AI often validates and builds on what users say, it can make distorted memories, conspiracy theories, or delusions feel more believable and emotionally real. Researchers warn that AI companions may be especially risky for isolated or vulnerable people seeking reassurance and connection.
- This 800-year-old Chinese exercise helps lower blood pressure naturallyon May 11, 2026
An ancient Chinese exercise routine may be just as powerful as a daily brisk walk for lowering blood pressure — without equipment, gyms, or intense workouts. In a major clinical trial, adults with stage 1 hypertension who practiced baduanjin, a gentle mind-body exercise combining slow movements, breathing, and meditation, saw meaningful drops in blood pressure within three months that lasted for an entire year.
PubMed, #vegan-diet –
- Iron Deficiency in Vegetarian Athletes: A Narrative Reviewon May 9, 2026
PURPOSE OF REVIEW: The increasing adoption of vegetarian dietary patterns among athletes (including lacto-ovo, lacto-, ovo-vegetarian, and vegan diets) has prompted growing interest in their potential effects on health and sports performance. Iron status remains one of the key nutritional concerns in this context, given the lower bioavailability of non-heme iron and the higher physiological demands of exercise. This review aims to synthesize and critically evaluate current evidence on the…
- Reduced interleukin-2 production and increased CREMα protein expression in vegetarians and vegans due to zinc deficiencyon May 9, 2026
Nutrition is a key determinant of health and may be regarded as a form of preventive medicine, as an adequate supply of vitamins, fats, proteins, and trace elements is essential for proper immune function. In recent decades vegetarian and vegan diets have become increasingly popular but may increase the risk of trace element deficiencies if not carefully planned. Zinc deficiency can impair immune responses and reduce resistance to infections. While previous research has mainly focused on […]
- Improving the protein quality of New Zealand vegan diets: an optimisation modelling approach incorporating energy constraints and diet acceptabilityon May 8, 2026
INTRODUCTION: Under consumption of certain indispensable amino acids (IAAs) is common in poorly planned vegan diets, but targeted dietary modifications through optimisation modelling can improve the overall protein adequacy and protein quality of these diets.
- Conditions for Knowledge and Application of Vegetarian/Vegan Diets Among Secondary School Students: A Cross-Sectional Studyon May 4, 2026
Background/Objectives: Knowledge of plant-based diets is gaining increasing significance in adolescents due to the growing popularity of vegetarian and vegan dietary patterns. To date, there has been limited research examining the level of awareness and understanding of these diets among secondary school students, as well as the factors influencing their knowledge. The aim of the study was to determine the prevalence of plant-based diets and to assess knowledge regarding these dietary […]
- A 2 year retrospective study of vegan patients and their pregnancy outcomes in a tertiary level Irish hospitalon April 30, 2026
CONCLUSION: The outcome in pregnancy for women with vegan and unrestricted diets was equivalent in our cohort. There is limited research on the consequences of vegan diets in pregnancy and further observational longitudinal studies are required for more robust data. Socioeconomic factors should be taken into consideration.
Random Posts –
Featured Posts –
Latest from PubMed, #plant-based diet –
- The association between the planetary health diet index (PHDI) and muscular dystrophies: A mediating role of phenotypic ageby Xiaomei Lin on May 12, 2026
To address the challenges posed by global aging and changing dietary habits, understanding the potential impact of healthy dietary patterns on diseases such as muscular dystrophies (MDs) and aging is crucial. The planetary health diet index (PHDI) is a dietary scoring system designed to balance human health and environmental sustainability by promoting the consumption of plant-based foods while reducing the intake of red meat, sugar, and highly processed foods. Additionally, phenotypic age is […]
- Effects of a Plant-Focused Diet on the Nutritional Status of Malnourished Patients Undergoing Peritoneal Dialysis in a Selected Hospital Care Setting: Protocol for an Open-Label, Parallel-Group,…by Qiao Qian Soon on May 12, 2026
CONCLUSIONS: This randomized controlled trial will provide clinical evidence on the nutritional and safety outcomes of a plant-focused diet in malnourished patients undergoing PD, addressing a major evidence gap in renal nutrition management.
- Host plant nutrition drives fitness outcomes in the cactus specialist Drosophila mettleriby Lidane Noronha on May 11, 2026
Organisms must navigate complex interactions with host plants, microbial communities, and environmental cues to ensure their survival and reproductive success when adapting to novel environments. Due to their ecological constraints, host plant specialists can be used to study how these interactions affect fitness due to their ecological constraints. In specialist species, such as cactophilic Drosophila, it remains unclear how feeding behavior, substrate composition, and microbial interactions…
- The Use of FTIR Spectra for Classifying Plant Items in a Vertebrate Herbivore’s Dietby Marcel Schäfer on May 10, 2026
Availability and quality of vegetation are critical factors influencing herbivore nutrition and population dynamics. Fourier-transform infrared spectroscopy (FTIR) offers a promising approach to analyze herbivore diets using spectral properties of phytochemicals to identify plant items. We evaluated the potential of FTIR to identify plant taxa and parts consumed by an herbivore species. Crop contents from 236 rock ptarmigan (Lagopus muta MONTIN) individuals from Iceland, collected over nine…
- Different Paths, Similar Pressures: Divergent Drivers of Genetic Diversity Despite Convergent Genomic Signatures of Selection in Response to Urban Intensity in Two Oligolectic Bee Speciesby Lucie M Baltz on May 9, 2026
Urbanisation is a pervasive form of anthropogenic environmental change and a driver of contemporary evolution. Yet, it remains unclear how demographic processes and environmentally associated genomic variation shape genomic patterns in cities and whether these responses depend on species-specific ecological traits. Here, we addressed this gap using whole-genome sequencing of two related, diet-specialised solitary bees (Andrena florea and Andrena vaga) that differ in dispersal-related traits,…
- Iron Deficiency in Vegetarian Athletes: A Narrative Reviewby Fernando Luna on May 9, 2026
PURPOSE OF REVIEW: The increasing adoption of vegetarian dietary patterns among athletes (including lacto-ovo, lacto-, ovo-vegetarian, and vegan diets) has prompted growing interest in their potential effects on health and sports performance. Iron status remains one of the key nutritional concerns in this context, given the lower bioavailability of non-heme iron and the higher physiological demands of exercise. This review aims to synthesize and critically evaluate current evidence on the…