Binge eating disorder- The psychology of hunger
In nature, there is no refined sugar or fat. Our brain had never been exposed to a combination of the two all at once forcing us into binge eating disorder.
Milos Pokimica
Written By: Milos Pokimica
Medically Reviewed by: Dr. Xiùying Wáng, M.D.
Updated October 12, 2023Eating for pleasure is nothing new. Binge eating disorder is nothing new. The ability to have excess food to binge is.
Binge eating disorder (BED) is a type of eating disorder that is now officially recognized as a diagnosis. It affects nearly 2% of the global population and can lead to additional health problems linked to diets, such as high cholesterol and diabetes.
Feeding and eating disorders are not solely about food, which is why they are classified as psychiatric disorders. People usually develop them to cope with a deeper issue or another psychological condition, such as anxiety or depression. The most common type of eating disorder in the United States is binge eating disorder. People suffering from binge eating disorder frequently feel out of control and consume a large amount of food at one time (called a binge). People with binge eating disorder, unlike those with other eating disorders, do not vomit their food after the binge. According to research, males and females experience binge eating disorder in equal proportions.
Overeating is a natural part of being human; we can overeat in social settings (e.g., Christmas lunch) or alone (e.g., a night in with Netflix and takeaway). Overeating occurs when a person eats past the point of being comfortably full, whether by choice or by accident. We may overeat if food is present, if the food we are eating is pleasurable, if we are bored or distracted, or if it soothes or comforts us (e.g., when feeling sad, overwhelmed, or after a tough day).
A binge is distinct from overeating and far more common. It is the intense desire to overeat that is felt repeatedly over time, accompanied by feelings of shame, guilt, and being out of control. Binge eating is extremely distressing and can impair a person’s ability to fully participate in all aspects of life (e.g., work or school, recreational activities, socializing, and relationships).
Binge eating disorder is defined as having at least three of the following symptoms while bingeing:
- Eating more quickly than usual
- Eating until uncomfortably full
- Eating large amounts of food when not hungry
- Eating alone to avoid embarrassment
- Feeling disgusted, depressed, or guilty afterward
Binge eating disorder is an addiction like any other addiction only in this case the illegal substance is highly palatable food. This is actually an addiction we all have but in some individuals, it might represent itself not just as obesity but as binge eating. To understand this addiction we have to understand how our brain evolved and understand that today we are maladapted to our environment in an evolutionary sense.
In nature, there is no free sugar or free fat. Energy is stored in complex whole-food packages and one or the other form. Nuts and seeds have their energy stored in the form of fat and grains for example in the form of complex sugars or carbohydrates, and they come with fiber and other substances. Our brain had never been exposed to refined sugar or fat before and especially never been exposed to a combination of the two in high doses all at once. For example, when we eat ice cream or milk chocolate, we have a sugar and fat combination that does not exist in nature. What happens in the brain is the same thing that happens when you inhale crack cocaine.
Crack cocaine itself is a refined product. Cocaine naturally occurs only in the coca plant. You cannot get high at that high level if you chew the leaves as Indian tribes do. It is a traditional stimulant to overcome hunger, fatigue, and thirst.
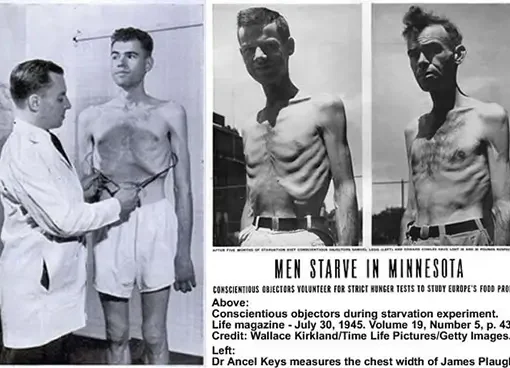
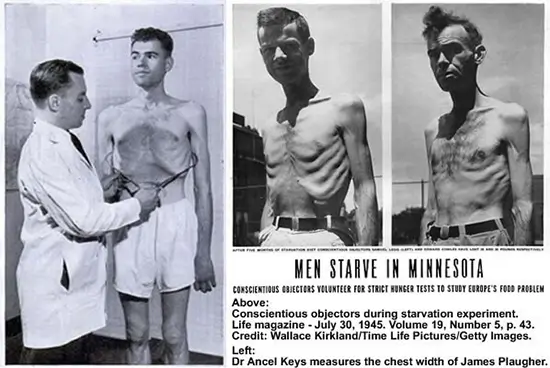
However, when we extract or in other words refine the cocaine or sugar or fat it is a different story. We can eat poppy seeds as much as we like but when we refine the opium and inject it into the vein or drink the poppy tea, well, here comes the magic dragon. In typical research involved with hunger and weight regulation, the focus was on so-called metabolic or homeostatic hunger. Metabolic hunger is driven by real physiological necessity and is most commonly identified with the rumblings of an empty stomach. By the 1980s researchers had mapped out all of the main hormones and neural connections responsible for metabolic hunger.
By the late 1990s, brain imaging studies and experiments with rodents had begun to reveal a second previously unknown biological pathway. This pathway was underlying the process of eating for pleasure. As I wrote before in the case of obesity standard regulatory system will tell the brain that we have fat deposits stored for an extended period and that we can endure little hunger. Overeating is a form of drug addiction.
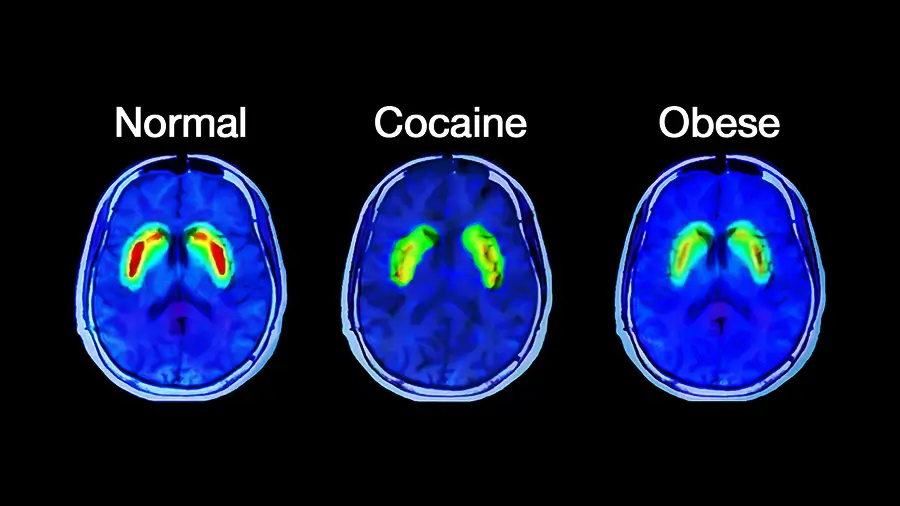
What was found was that extremely sweet or fatty food that we have today but were not present in nature, captivate the brain reward circuit in much the same way that cocaine and gambling can do. Even just seeing the food will trigger the brain’s response. As quickly as such food meets the tongue, taste buds give signals to different areas of the brain. That will result in a response that will trigger the release of the neurochemical dopamine. Frequently overeating highly palatable foods saturate the cerebellum with a significant amount of dopamine that forces the brain to ultimately adjusts by desensitizing itself, decreasing the number of cellular receptors that identify and respond to the neurochemical.
Having a high and constant dopamine level is a form of stimulus that is over-excessive, something called supernormal stimuli. It is a term that evolutionary biologists apply to represent the stimulus that will evoke a response more significant than the stimulus for which it evolved, even if it is artificial. The food industry uses it all the time almost in every possible way they can think of. They even try to link emotional responses and feelings of social acceptance and well-being with supernormal stimuli.
Consequently, as a resistance build-up, people may in truth, proceed to gorge as a process of recollecting or even preserving a sense of well-being. This is possibly the reason why the downregulation of leptin receptors in the brain happens also.
There was a series of research done from 2007 to 2011, at the University of Gothenburg in Sweden. They proved that the release of ghrelin (the hunger hormone) by the abdomen immediately enhances the discharge of dopamine in the brain’s award circuit (Anderberg et al., 2016). This is a significant finding. They also discovered that medications that prevent ghrelin from binding to neurons restrain the tendency for overeating in people who are obese.
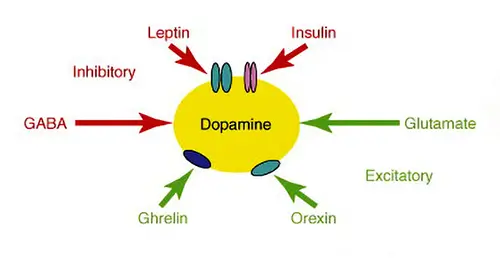
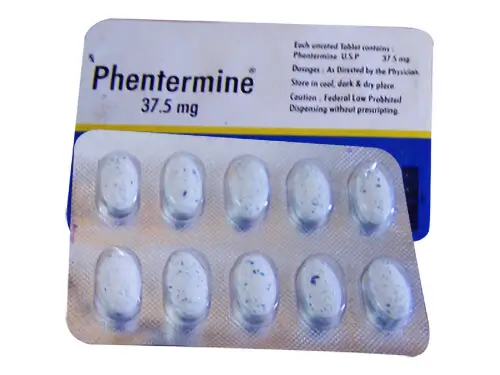
Under normal conditions, leptin and insulin suppress the release of dopamine. In theory, this should reduce the sense of pleasure as a meal continues. Recent rodent studies suggest that the brain stops responding to these hormones as the amount of fatty tissue in the body increases (Massadi et al., 2019). Thus, continued eating keeps the brain awash in dopamine even as the threshold for pleasure keeps going up. A form of maladaptation to our current environment and way of eating and living. If we switch the stimuli from food to cocaine or nicotine or caffeine, we can suppress the hunger drive. Alternatively, also vice versa. If we stop smoking appetite goes up. Tobacco use was linked to hunger-suppressing effects even among Pre-Columbian indigenous Americans. Cigarette smoking for weight loss might not be a good idea, because we will swap one addiction for another. You can try extracted nicotine in products like chewing gum or electronic cigarettes with a caffeine combination. There is, for example, particular drugs that target the brain hunger center for lowering appetite like Belviq, Contrave, Saxenda, Phentermine, and Qsymia. Phentermine is an amphetamine. Regular “speed” can work also. The anti-seizure drug Topamax for epilepsy and migraine headaches lowers the appetite and is registered to treat binge eating disorders. If everything else fails, there are seven weight loss surgeries registered so far, from cutting, and stapling to ballooning. All because of supernormal stimuli of refined food.
There is a group of sensitive individuals that will respond excessively to delicious foods. They would have an excessive response in the brain reward circuit that will dramatically alter their brain chemistry. An overstimulated brain reward circuit will override any self-control mechanism so that willpower will rarely if ever be sufficient to force them to resist eating those foods once they are around creating a binge eating disorder. Researchers at The Scripps Research Institute in Jupiter, Florida found that in rats that have been given unrestricted access to high-calorie foods, their brains showed neurological changes in their reward circuit (Johnson et al., 2010).
It was the first study that showed that the neurological mechanism that drives people into drug addiction is also driving the compulsion for overeating, pushing people into obesity.
High-calorie foods, in this case, were sausage, bacon, cheesecake, and chocolate. Some of the rats were given only one hour a day to feast on high-fat foods, while others had unlimited access 24 hours a day. Both groups were given access to a typical, healthy lab rat chow food. The one group that possessed infinite access to high-calorie food ate little to none of the standard bland low-calorie chow alternatives. They quickly had grown obese because they eat as much as they could, about twice the amount of calories as the control.
The big surprise was that even the rats that had limited access to junk food did their best to keep up. During that one hour, they ate as much as they can with no stopping. They managed to consume, on average, 66% of their daily calories in the course of that one single hour per day and quickly developed a pattern of compulsive binge eating disorder. It was also observed that a group of obese rats with unlimited access to junk food had shown a severely increased threshold for reward levels. The same thing happens with drug addiction. After showing that obese rats had clear addiction-like food-seeking behaviors and that an increased threshold for reward levels is forcing them to seek more and more to reach the same level of reward the researchers investigated underlying neurological mechanisms that are responsible for these changes.
There is a specific receptor in the brain known to play a significant role in vulnerability to drug addiction, the dopamine D2 receptor. In the brain, there are neurotransmitters like dopamine. Dopamine is a feel-good chemical that will get released when we have some pleasurable experience like sex or food. The D2 receptor responds to dopamine. Cocaine, for example, is a drug that increases dopamine levels in the brain by blocking its retrieval. Overstimulation of the dopamine receptors with any supernormal stimuli will eventually lead to neural adaptation in the form of downregulation of the receptors. Also, this was shown in the study too. Levels of the D2 dopamine receptors were significantly reduced in the brains of obese animals. The same thing happens to drug addicts. To determent the level of influence of dopamine in the rats eating behavior, a virus was inserted into the brains of a test group of animals to knock out their dopamine D2 receptors. Addiction-like behavior happened almost instantly. The next day their brains changed into a state that was consistent with an animal that had been overeating for several weeks. Also, the animals had become compulsive in their eating behaviors and developed binge eating disorders. The research that took three years to finish confirms the addictive properties of junk food.
Animals binge-eating lipids and animals binge-eating sugars experience different physiological effects, but the most substantial impact can be brought by the combination of neural effects from both of these ingredients. Actually, the most desired food for the lab rats appeared to be a food item with the highest combination of fat and sugar: cheesecake.
References:
- Anderberg, R. H., Hansson, C., Fenander, M., Richard, J. E., Dickson, S. L., Nissbrandt, H., Bergquist, F., & Skibicka, K. P. (2016). The Stomach-Derived Hormone Ghrelin Increases Impulsive Behavior. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology, 41(5), 1199–1209. https://doi.org/10.1038/npp.2015.297
- Al Massadi, O., Nogueiras, R., Dieguez, C., & Girault, J. A. (2019). Ghrelin and food reward. Neuropharmacology, 148, 131–138. https://doi.org/10.1016/j.neuropharm.2019.01.001
- Johnson, P. M., & Kenny, P. J. (2010). Dopamine D2 receptors in addiction-like reward dysfunction and compulsive eating in obese rats. Nature neuroscience, 13(5), 635–641. https://doi.org/10.1038/nn.2519
- Palmiter R. D. (2007). Is dopamine a physiologically relevant mediator of feeding behavior?. Trends in neurosciences, 30(8), 375–381. https://doi.org/10.1016/j.tins.2007.06.004
- Obradovic, M., Sudar-Milovanovic, E., Soskic, S., Essack, M., Arya, S., Stewart, A. J., Gojobori, T., & Isenovic, E. R. (2021). Leptin and Obesity: Role and Clinical Implication. Frontiers in endocrinology, 12, 585887. https://doi.org/10.3389/fendo.2021.585887
- Crujeiras, A. B., Carreira, M. C., Cabia, B., Andrade, S., Amil, M., & Casanueva, F. F. (2015). Leptin resistance in obesity: An epigenetic landscape. Life sciences, 140, 57–63. https://doi.org/10.1016/j.lfs.2015.05.003
- Peng, J., Yin, L., & Wang, X. (2021). Central and peripheral leptin resistance in obesity and improvements of exercise. Hormones and behavior, 133, 105006. https://doi.org/10.1016/j.yhbeh.2021.105006
Related Posts
Do you have any questions about nutrition and health?
I would love to hear from you and answer them in my next post. I appreciate your input and opinion and I look forward to hearing from you soon. I also invite you to follow us on Facebook, Instagram, and Pinterest for more diet, nutrition, and health content. You can leave a comment there and connect with other health enthusiasts, share your tips and experiences, and get support and encouragement from our team and community.
I hope that this post was informative and enjoyable for you and that you are prepared to apply the insights you learned. If you found this post helpful, please share it with your friends and family who might also benefit from it. You never know who might need some guidance and support on their health journey.
– You Might Also Like –

Learn About Nutrition
Milos Pokimica is a doctor of natural medicine, clinical nutritionist, medical health and nutrition writer, and nutritional science advisor. Author of the book series Go Vegan? Review of Science, he also operates the natural health website GoVeganWay.com
Medical Disclaimer
GoVeganWay.com brings you reviews of the latest nutrition and health-related research. The information provided represents the personal opinion of the author and is not intended nor implied to be a substitute for professional medical advice, diagnosis, or treatment. The information provided is for informational purposes only and is not intended to serve as a substitute for the consultation, diagnosis, and/or medical treatment of a qualified physician or healthcare provider.NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY SEEKING MEDICAL TREATMENT BECAUSE OF SOMETHING YOU HAVE READ ON OR ACCESSED THROUGH GoVeganWay.com
NEVER APPLY ANY LIFESTYLE CHANGES OR ANY CHANGES AT ALL AS A CONSEQUENCE OF SOMETHING YOU HAVE READ IN GoVeganWay.com BEFORE CONSULTING LICENCED MEDICAL PRACTITIONER.
In the event of a medical emergency, call a doctor or 911 immediately. GoVeganWay.com does not recommend or endorse any specific groups, organizations, tests, physicians, products, procedures, opinions, or other information that may be mentioned inside.
Editor Picks –
Milos Pokimica is a health and nutrition writer and nutritional science advisor. Author of the book series Go Vegan? Review of Science, he also operates the natural health website GoVeganWay.com
Latest Articles –
Top Health News — ScienceDaily
- This common amino acid helped mice survive deadly inflammationon June 1, 2026
A Salk Institute study found that a simple dietary amino acid, methionine, dramatically improved survival in mice facing severe infections and inflammatory conditions. Rather than directly targeting the immune system, methionine boosted kidney filtration, helping the body flush out excess inflammatory molecules that can cause tissue damage, brain dysfunction, wasting, and death.
- This drug delayed rheumatoid arthritis for years after treatment endedon June 1, 2026
A promising new study suggests rheumatoid arthritis may not be as inevitable as once thought for people at high risk. Researchers found that just one year of treatment with the immune-targeting drug abatacept delayed the onset of rheumatoid arthritis by up to four years, with benefits lasting long after treatment ended.
- The forgotten organ that could predict how long you liveon June 1, 2026
A long-overlooked organ may hold surprising clues to healthy aging and cancer survival. Researchers at Mass General Brigham used AI to analyze CT scans from tens of thousands of adults and found that people with healthier thymuses—a small immune-system organ once thought to become largely irrelevant after childhood—lived longer and had substantially lower risks of heart disease, cancer, and death.
- Scientists found the hidden switch fueling alzheimer’s brain inflammationon May 31, 2026
Scientists at Scripps Research have uncovered a molecular “switch” that appears to fuel the damaging brain inflammation seen in Alzheimer’s disease. They found that a protein called STING becomes chemically altered in a way that keeps the brain’s immune system stuck in overdrive, harming the connections between nerve cells.
- Why cancer spreads more in middle age than in old ageon May 31, 2026
Melanoma may not become steadily more dangerous with age as scientists once assumed. In a surprising discovery, researchers found that cancer spread was lowest in young mice, surged in middle-aged mice, and then dropped again in very old mice. The key appears to be a special type of immune cell that helps keep cancer dormant and prevents it from spreading.
- Intermittent fasting triggers surprising changes in the brainon May 31, 2026
Losing weight may involve rewiring the gut and the brain at the same time. In a study of obese adults, an intermittent fasting-style diet led to significant weight loss, healthier metabolic markers, and notable shifts in gut bacteria. Brain scans also revealed changes in regions tied to appetite, cravings, and self-control. The results suggest the gut microbiome and brain may work together to influence weight-loss success.
- Omega-3 fish oil shows promise against type 2 diabeteson May 31, 2026
A new study suggests fish oil may help reduce insulin resistance even in people who aren’t obese. In diabetic rats, omega-3 supplementation improved blood sugar levels, cholesterol, and inflammation by shifting immune cells into a more anti-inflammatory mode.
PubMed, #vegan-diet –
- Editorial: Recent insights in vegetarian nutritionon June 1, 2026
No abstract
- Pet food choices in transition: how owner demographics and diets influence pet food selection and the acceptance of alternative protein sources in pet feedingon June 1, 2026
Given the increasing interest in alternative protein sources and growing ethical awareness in nutrition, this large-scale survey (n = 8,823) investigated the feeding practices of dog and cat owners in mainly German-speaking countries. The aim was to assess preferences, feeding habits, and the acceptance of novel protein sources such as plant- and insect-based pet foods. The results showed that conventional meat-based diets remained predominant (i.e., 53.05% daily feeding of meat-based dry […]
- Environmental Footprint of a Low-Fat Vegan Diet in People With Type 1 Diabetes: A Secondary Analysis of a Randomized Clinical Trialon May 29, 2026
A 12-wk randomized clinical trial found that adults with type 1 diabetes on a low-fat, vegan diet (n = 29) showed greater improvements in insulin sensitivity compared with a portion-controlled diet (n = 29). This secondary analysis calculates the greenhouse gas emissions (GHGEs) and cumulative energy demand (CED) of both diets by linking 3-d dietary records to external data sources. A repeated-measures analysis of variance was performed unadjusted and adjusted for change in energy intake. […]
- Protein intake and preservation of function in old age : Current evidence and present research gapson May 28, 2026
In the past, large observational cohort studies suggested that a higher protein intake might slow the age-associated loss of muscle mass and muscle strength. This observation led to the conclusion that a higher protein intake may contribute to a preservation of function and to the prevention of sarcopenia. Therefore, the German Nutrition Society increased their recommendation for daily protein intake in adults aged ≥ 65 years from 0.8 to 1.0 g/kg body weight (estimated value); however, […]
- Flexitarian dietary patterns and neuropsychiatric multimorbidity among the oldest-old in Chinaon May 27, 2026
CONCLUSION: In this nationally representative sample of older Chinese adults, flexitarian dietary patterns were not associated with better neuropsychiatric health and were instead linked to higher odds of depression, cognitive impairment, and their co-occurrence. These results suggest that plant-forward diets in the oldest-old should place greater emphasis on overall dietary quality and nutrient adequacy.
Random Posts –
Featured Posts –
Latest from PubMed, #plant-based diet –
- Adherence to the EAT-Lancet diet and neuropsychiatric disorders: a systematic review and meta-analysisby Yuhao Wang on June 1, 2026
Neuropsychiatric disorders (NPDs) are a leading cause of disability worldwide. The predominantly plant-based EAT-Lancet diet has been proposed to confer neuropsychiatric benefits, yet evidence remains limited. This study synthesized associations between adherence to the EAT-Lancet diet and neuropsychiatric outcomes. We searched PubMed, Web of Science, Embase, Scopus, and ProQuest Dissertations and Theses Global through September 4, 2025. Observational studies reporting associations between…
- The Association of Maternal Dietary Patterns With Asthma and Wheeze Diagnosis in Canadian Childrenby Fazle Rabbi on June 1, 2026
Asthma affects over 850,000 Canadian children under 14, ranking among the top chronic childhood diseases. Prenatal dietary factors are hypothesised to influence its development. We examined associations between maternal prenatal dietary patterns and childhood asthma/wheeze in the CHILD cohort. Principal component analysis derived three dietary patterns (plant-based, Western, balanced) from food frequency questionnaires. Logistic regression and generalised estimating equations (GEE) models…
- Editorial: Recent insights in vegetarian nutritionby Luciana Baroni on June 1, 2026
No abstract
- Pet food choices in transition: how owner demographics and diets influence pet food selection and the acceptance of alternative protein sources in pet feedingby Ammelie Godglück on June 1, 2026
Given the increasing interest in alternative protein sources and growing ethical awareness in nutrition, this large-scale survey (n = 8,823) investigated the feeding practices of dog and cat owners in mainly German-speaking countries. The aim was to assess preferences, feeding habits, and the acceptance of novel protein sources such as plant- and insect-based pet foods. The results showed that conventional meat-based diets remained predominant (i.e., 53.05% daily feeding of meat-based dry […]
- Plant-Based Diet and Risk of Sepsis: A 16-Year Follow-Up Studyby Shaokang Xu on June 1, 2026
CONCLUSIONS: Adherence to a healthy plant-based diet was associated with a lower risk of sepsis, whereas adherence to an unhealthy plant-based diet was associated with an increased risk, independently of other traditional risk factors. The associations may be partly mediated through metabolic and inflammatory pathways. These findings underscore the role of high-quality plant-based diet in sepsis prevention.
- Cross-sectional association between adherence to a planetary health diet and self-reported infertility in U.S. women (NHANES 2013-2018)by Qiao Li on May 30, 2026
The relationship between dietary patterns aligned with the EAT-Lancet reference diet, which promotes both human and planetary health, and female infertility remains unexplored. This study aimed to investigate the association between adherence to the plant-based diet index (PHDI) and infertility among United States women of reproductive age. We conducted a cross-sectional analysis of data from the 2013 to 2018 National Health and Nutrition Examination Survey. The study included 3105 women aged […]