Cooked meat bacteria endotoxemia- Inflammation and diet
Are humans omnivores in a true anatomical sense? There is a fundamental difference in the way the digestive tract works in plant vs meat-eating species.
Milos Pokimica
Written By: Milos Pokimica
Medically Reviewed by: Dr. Xiùying Wáng, M.D.
Updated June 9, 2023The emerging role of chronic inflammation in modern society’s major chronic diseases has sparked research into the impact of nutrition and dietary patterns on inflammatory status. The majority of human studies have linked dietary intake to systemic inflammation markers such as high-sensitivity C-reactive protein (HS-CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-).
Significant dietary influences have been established for glycemic index (GI) and load (GL), fiber, fatty acid composition, magnesium, carotenoids, and flavonoids. Whole food plant-based diet or even a traditional Mediterranean dietary pattern, which typically has a high ratio of monounsaturated (MUFA) to saturated (SFA) fats and ω-3 to ω-6 polyunsaturated fatty acid (PUFAs) and supplies an abundance of fruits, vegetables, legumes, and grains, has shown anti-inflammatory effects when compared with typical North American and Northern European dietary patterns in most observational and interventional studies. There is a wide range of factors that influence inflammation caused by diet but a whole food antioxidant-rich, nutrient-rich diet may become the diet of choice for diminishing chronic inflammation in clinical practice.
Prolonged low-grade inflammation is linked to increased oxidative stress and altered glucose and lipid metabolism in fat (adipose) cells, muscle, and the liver. As a result, research indicates that certain dietary components can influence these key inflammatory pathways.
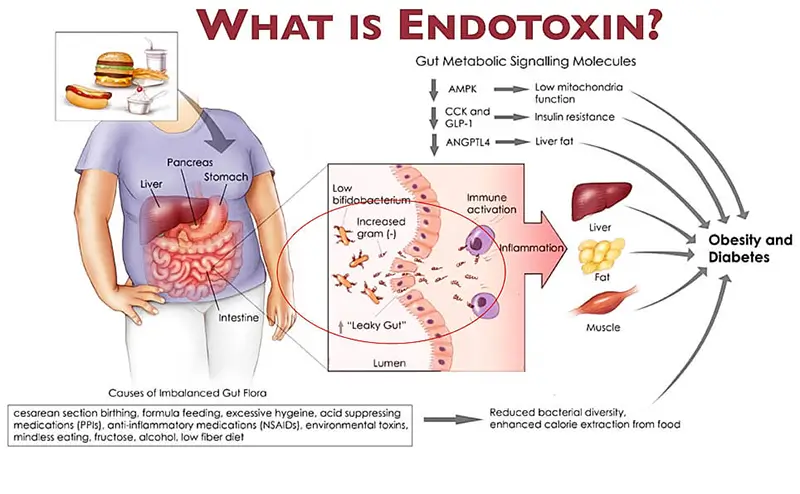
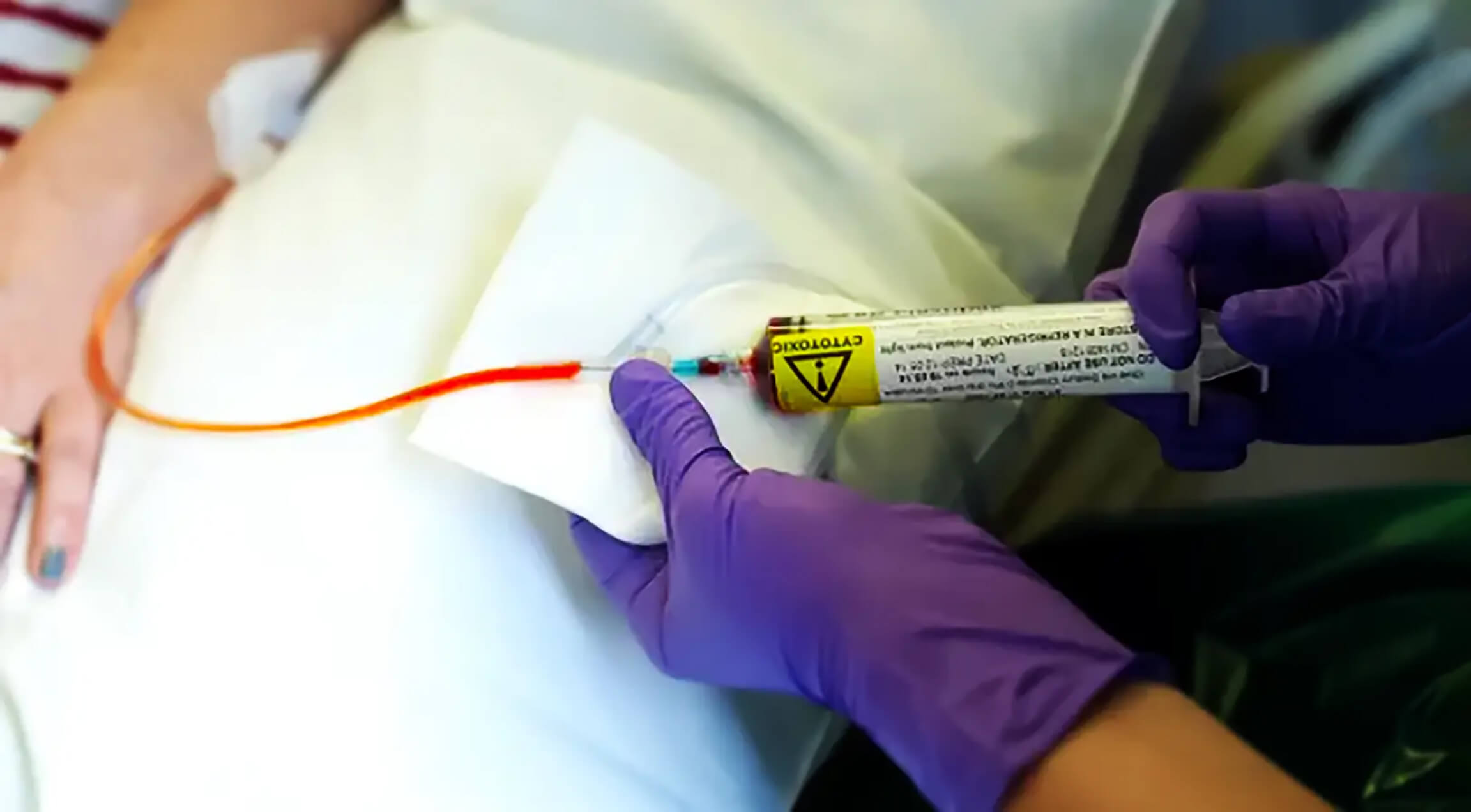
One of the factors that creates inflammation spikes after animal product consumption is a process known as endotoxemia. `Diet-induced metabolic endotoxemia has been proposed as a major root cause of inflammation, and these pathways appear to be detrimental to healthy aging.
We as humans, unlike carnivores species, have very low resistance filters meaning any live bacteria we eat will be creating inflammation, and diet can kill us if bacteria is dangerous. We cannot eat uncooked meat. Carnivorous animals have extremely corrosive bile acids that are able to kill any living microorganism and their digestive system is practically sterile. We as any other plant eater have mild bile acid and low resistance filters and have to cook meat and any other food item that has the potential to spread an infectious disease. For example, pasteurization is mandatory.
What people don’t understand is that even if we do cook meat we do not magically dematerialize all of the bacteria that were present in there. We only kill them by heat but they are still in there. Microorganisms are still in the meat just dead. They will not pose any risk of infection anymore.
But that does not mean that they don’t pose a risk anymore.
Even dead non-probiotic bacteria do count as toxins.
Some of the world’s most toxic substances are these dead meat bacteria endotoxins.
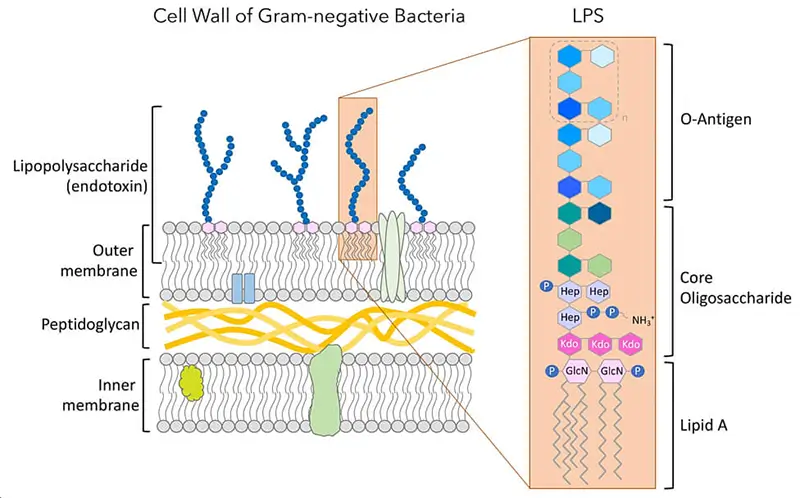
These substances known as endotoxins (Greek éndon within; cognate with Old Irish ind-) are thermally (250C) and chemically stable and extremely toxic. Endotoxin is a complex lipopolysaccharide (LPS) found in the outer cell membrane of gram-negative bacteria (E.coli, Salmonella typhi, Shigella).
Bacteria shed endotoxins in large amounts upon cell death creating an endotoxemia state in the body. Meaning, the bacteria can be dead or cooked for a long time, but their endotoxins are still there. Endotoxins are chemically very stable and can withstand our body’s best attempts at acid and enzyme degradation. One of the leading causes of hundreds of studies that display enlarged inflammation from animal foods, but not from most plant foods, maybe is a consequence of a toxic load of dead bacteria endotoxins in animal products. These bacteria shed endotoxins after death and then when we eat them they are absorbed into our system, leading to the endotoxemia inflammation we see after egg, meat, and dairy consumption, as well.
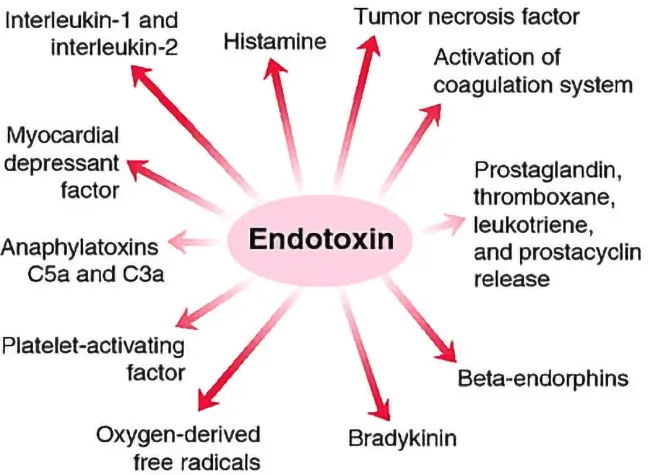
This would cause damage to our internal organs and the entire body and will increase the chances of chronic diseases (Ghosh et al., 1993).
If we already have an autoimmune disease such as atherosclerosis, for example, this will just agitate our immune system even worse and would create even more of an immune response (Stoll et al., 2004).
Here is one study that discovered a link between endotoxin exposure and diabetes type 2 (Harte et al., 2012).
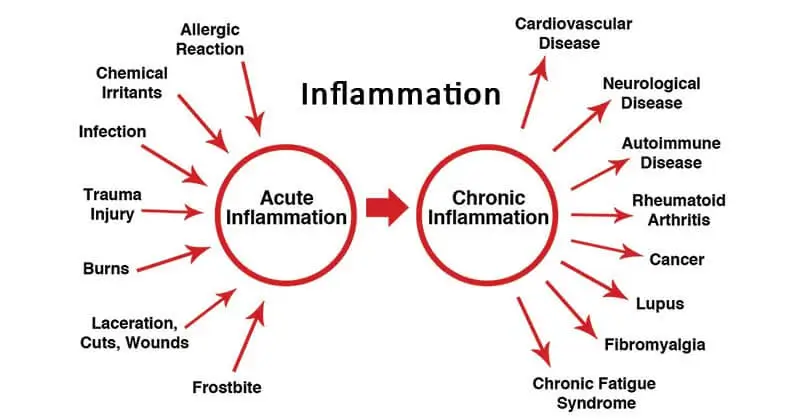
What a low level of chronic endotoxemia inflammation does is that it causes damage like any other inflammation just in a prolonged period. What that translates to is faster and more noticeable DNA damage, a higher mortality rate from chronic diseases, and decreased longevity.
In contrast, plant foods do not show this trait, and actual consumption is correlated with the anti-inflammatory reaction after a meal because of the antioxidants and other anti-inflammatory phytochemicals. It would be interesting to see how much inflammation meat consumption causes in carnivorous species. So far I was unable to find research that looks into dead meat bacteria endotoxemia exposure in carnivorous species. This could be potentially interesting because if meat causes no inflammation in carnivorous animals, we might look at a way how to lower the same inflammation in our own bodies.
Consumption of meat, therefore, is associated with an increase in inflammation even if we disregard the risk of live infectious bacteria. This mechanism is natural and normal, and all of the carnivorous species had it to some extent but are more adept at coping with it.
A fresh hamburger contains approximately a hundred million bacteria per quarter pounder. Eating meals high in bacterial endotoxins could develop mild but systemic inflammatory episodes that predispose subjects to the development of chronic diseases.
The animal fat that comes in the same package may play a role in the pathogenesis of this after-meal inflammation. Endotoxins hold a powerful attraction for saturated fat, so they stick to it and then get absorbed through the gut wall and into the bloodstream (Erridge, 2011).
Would this happen if we eat food that is high in saturated fat from plant origin? It would, but the difference is that there are no high levels of these toxins in plant-based foods. For example, cocoa has a high fat content. It is one of the plants that has energy stored in a form of saturated fat, the same fat that is found in the animal kingdom. But cocoa also has a large number of antioxidants and in studies always decreases the level of C-reactive protein in subjects (a marker for inflammation) (Erridge et al., 2007), (Herieka et al., 2014).
The high antioxidant content of cocoa prevails and is able to neutralize the pro-inflammatory effects of endotoxins that are not present in the plants in high numbers, to begin with (Gu et al., 2014).
The problem with meat is a high concentration of bacteria. This means that eating a standard Western diet rich in animal protein and refined sugar and fat will require a much higher level of antioxidants to negate the bad pro-inflammatory effects.
The question will be where can we use these findings and can we diminish the bed proinflammatory effects of high animal protein meals with antioxidant-rich food. In other words, can we still eat meat but also add some high-antioxidant vegetables or fruits to the same meal to avoid the risk (Burton-Freeman, 2010).
There was a large number of studies done on a topic and the conclusion is yes, we can, but only to some extent. Avoidance of toxin exposure is our primary goal. If you really have to eat animal products then at least incorporate an adequate amount of anti-inflammatory food sources and calculate your optimal ORAC (Oxygen radical absorbance capacity) intake. You can find ORAC values here (ORAC Values). This would not completely negate the toxicity of dead meat bacteria endotoxemia exposure. These toxins are very potent and hard to detoxify. There are genetically susceptible individuals that have a harder time detoxifying these compounds. Antioxidant-rich food will lower the risk to a relevant degree and my advice is to optimize the antioxidant intake.
The best course of action would be to have a whole food plant-based diet that has an optimal level of ORAC units and a wide range of proinflammatory food sources with an adequate level of all essential micronutrients.
This is what the British Journal of Nutrition has to say about it.
“Postprandial (fed) state is a pro-oxidant state. The postprandial period is a time of active oxidative metabolism and formation of ROS (free radicals). There is increasing evidence that the postprandial state is an important contributing factor to chronic disease. Two main questions are posed: first, what is the role of plant foods, specifically fruits rich in complex and simple phenolic compounds in postprandial metabolic management; and second, does the evidence support consuming these fruits with meals as a practical strategy to preserve health and lower risk for disease? The collected data suggest that consuming phenolic-rich fruits increases the antioxidant capacity of the blood, and when they are consumed with high fat and carbohydrate ‘pro-oxidant and pro-inflammatory’ meals, they may counterbalance their negative effects. Given the content and availability of fat and carbohydrate in the Western diet, regular consumption of phenolic-rich foods, particularly in conjunction with meals, appears to be a prudent strategy to maintain oxidative balance and health.“
References:
- Ghosh, S., Latimer, R. D., Gray, B. M., Harwood, R. J., & Oduro, A. (1993). Endotoxin-induced organ injury. Critical care medicine, 21(2 Suppl), S19–S24. https://doi.org/10.1097/00003246-199302001-00005
- Stoll, L. L., Denning, G. M., & Weintraub, N. L. (2004). Potential role of endotoxin as a proinflammatory mediator of atherosclerosis. Arteriosclerosis, thrombosis, and vascular biology, 24(12), 2227–2236. https://doi.org/10.1161/01.ATV.0000147534.69062.dc
- Harte, A. L., Varma, M. C., Tripathi, G., McGee, K. C., Al-Daghri, N. M., Al-Attas, O. S., Sabico, S., O’Hare, J. P., Ceriello, A., Saravanan, P., Kumar, S., & McTernan, P. G. (2012). High fat intake leads to acute postprandial exposure to circulating endotoxin in type 2 diabetic subjects. Diabetes care, 35(2), 375–382. https://doi.org/10.2337/dc11-1593
- Erridge C. (2011). The capacity of foodstuffs to induce innate immune activation of human monocytes in vitro is dependent on food content of stimulants of Toll-like receptors 2 and 4. The British journal of nutrition, 105(1), 15–23. https://doi.org/10.1017/S0007114510003004
- Erridge, C., Attina, T., Spickett, C. M., & Webb, D. J. (2007). A high-fat meal induces low-grade endotoxemia: evidence of a novel mechanism of postprandial inflammation. The American journal of clinical nutrition, 86(5), 1286–1292. https://doi.org/10.1093/ajcn/86.5.1286
- Herieka, M., & Erridge, C. (2014). High-fat meal induced postprandial inflammation. Molecular nutrition & food research, 58(1), 136–146. https://doi.org/10.1002/mnfr.201300104
- Gu, Y., Yu, S., Park, J. Y., Harvatine, K., & Lambert, J. D. (2014). Dietary cocoa reduces metabolic endotoxemia and adipose tissue inflammation in high-fat fed mice. The Journal of nutritional biochemistry, 25(4), 439–445. https://doi.org/10.1016/j.jnutbio.2013.12.004
- Burton-Freeman B. (2010). Postprandial metabolic events and fruit-derived phenolics: a review of the science. The British journal of nutrition, 104 Suppl 3, S1–S14. https://doi.org/10.1017/S0007114510003909
Related Posts
Do you have any questions about nutrition and health?
I would love to hear from you and answer them in my next post. I appreciate your input and opinion and I look forward to hearing from you soon. I also invite you to follow us on Facebook, Instagram, and Pinterest for more diet, nutrition, and health content. You can leave a comment there and connect with other health enthusiasts, share your tips and experiences, and get support and encouragement from our team and community.
I hope that this post was informative and enjoyable for you and that you are prepared to apply the insights you learned. If you found this post helpful, please share it with your friends and family who might also benefit from it. You never know who might need some guidance and support on their health journey.
– You Might Also Like –

Learn About Nutrition
Milos Pokimica is a doctor of natural medicine, clinical nutritionist, medical health and nutrition writer, and nutritional science advisor. Author of the book series Go Vegan? Review of Science, he also operates the natural health website GoVeganWay.com
Medical Disclaimer
GoVeganWay.com brings you reviews of the latest nutrition and health-related research. The information provided represents the personal opinion of the author and is not intended nor implied to be a substitute for professional medical advice, diagnosis, or treatment. The information provided is for informational purposes only and is not intended to serve as a substitute for the consultation, diagnosis, and/or medical treatment of a qualified physician or healthcare provider.NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY SEEKING MEDICAL TREATMENT BECAUSE OF SOMETHING YOU HAVE READ ON OR ACCESSED THROUGH GoVeganWay.com
NEVER APPLY ANY LIFESTYLE CHANGES OR ANY CHANGES AT ALL AS A CONSEQUENCE OF SOMETHING YOU HAVE READ IN GoVeganWay.com BEFORE CONSULTING LICENCED MEDICAL PRACTITIONER.
In the event of a medical emergency, call a doctor or 911 immediately. GoVeganWay.com does not recommend or endorse any specific groups, organizations, tests, physicians, products, procedures, opinions, or other information that may be mentioned inside.
Editor Picks –
Milos Pokimica is a health and nutrition writer and nutritional science advisor. Author of the book series Go Vegan? Review of Science, he also operates the natural health website GoVeganWay.com
Latest Articles –
Top Health News — ScienceDaily
- Scientists say a daily multivitamin may help slow agingon May 14, 2026
A daily multivitamin may help slow biological aging, according to researchers studying older adults in a large clinical trial. After two years, participants taking multivitamins showed slower aging in several DNA-based “epigenetic clocks,” with the effect equal to about four months less biological aging. People who started out biologically older than their actual age appeared to benefit the most. The findings hint that a simple supplement could play a role in healthier aging.
- Who are the Japanese? Huge DNA discovery rewrites historyon May 14, 2026
Scientists analyzing the genomes of thousands of people across Japan discovered evidence for a previously overlooked third ancestral group, challenging the long-accepted “dual origins” theory. The newly identified ancestry appears linked to the ancient Emishi people of northeastern Japan. Researchers also uncovered inherited Neanderthal and Denisovan DNA connected to conditions like diabetes, heart disease, and cancer.
- New psychedelic-like drugs could treat depression without making you tripon May 14, 2026
UC Davis researchers created brand-new psychedelic-like compounds by shining UV light on amino acid-based molecules. These compounds activated key serotonin receptors tied to brain plasticity and mental health benefits, but surprisingly did not cause hallucination-like behavior in animal tests. Scientists say the discovery could lead to future treatments for depression, PTSD, and addiction without the intense psychedelic experience.
- This daily habit could lower dementia risk by 35%, scientists sayon May 13, 2026
A huge long-term study found that drinking two to three cups of coffee a day was linked to a much lower risk of dementia, especially before age 75. Researchers say caffeine may help keep brain cells active while reducing inflammation and harmful plaque buildup associated with Alzheimer’s disease. But more coffee wasn’t better — the protective effect appeared to level off after moderate intake.
- Scientists discover a mysterious silicone pollutant that may be everywhereon May 13, 2026
Researchers have uncovered unexpectedly high levels of silicone-based pollutants called methylsiloxanes floating through the atmosphere across cities, rural regions, and even forests. Much of the pollution appears to come from vehicle emissions, likely linked to engine oil additives that survive combustion and escape into the air. Scientists say humans may inhale more of these compounds daily than other notorious pollutants like PFAS or microplastics.
- Your “um” and pauses could reveal early dementia riskon May 13, 2026
The little pauses, “ums,” and moments when you struggle to find the right word may reveal far more about your brain than anyone realized. Researchers discovered that everyday speech patterns are closely tied to executive function — the mental system that powers memory, planning, focus, and flexible thinking. By using AI to analyze natural conversations, the team found they could predict cognitive performance with surprising accuracy, potentially opening the door to simple speech-based […]
- A rare cancer-fighting plant compound has been decodedon May 13, 2026
Scientists at UBC Okanagan have uncovered how plants produce mitraphylline, a rare natural compound with promising anti cancer potential. The team identified two enzymes that work together to build the molecule’s unusual twisted structure, solving a mystery that had puzzled researchers for years. Because mitraphylline appears only in tiny amounts in tropical plants like kratom and cat’s claw, the discovery could make it far easier to produce sustainably in the future.
PubMed, #vegan-diet –
- Severe Hypocalcaemia with Elevated PTH and Normal Vitamin D: A Diagnostic Pitfall due to Chronic Negative Calcium Balance in a Vegan Patienton May 14, 2026
CONCLUSION: A chronic negative calcium balance is an under-recognised cause of secondary hyperparathyroidism. Measurement of urinary calcium is a key diagnostic tool in these patients.
- Plant-based diets for human health with implications for cardiometabolic health, gut microbiome, and nutritional adequacyon May 14, 2026
Plant-based diets have gained considerable interest in recent times due to their perceived health and environmental benefits. However, the term “plant-based diet” refers to a broad range of diets with a wide range of differences in food quality and nutritional content. This article aims to summarize the available evidence regarding the health and environmental impacts of plant-based diets, including new trends and issues. Epidemiological studies, RCTs, and life cycle assessment studies were…
- DNA Damage Across Dietary Patterns: A Comet Assay Study in Vegans and Omnivoreson May 13, 2026
Plant-based diets are generally associated with a reduced risk of chronic diseases; however, the relationship between a vegan diet and genome integrity remains insufficiently characterized. In this cross-sectional study, we assessed primary DNA damage in peripheral blood cells of vegans and omnivores. A total of 62 apparently healthy adults were included: 31 vegans (median vegan diet duration 4.5 years) and 31 omnivores matched for sex and smoking status. DNA damage was assessed using the…
- The Role of Microbiome and Diet on Disease Activity and Immune-Inflammatory Status in Rheumatoid Arthritison May 13, 2026
Rheumatoid arthritis (RA) is a chronic inflammatory disease of autoimmune background and unknown etiology. The importance of genetic factors in RA development is well-established. Environmental factors have also been extensively researched in relation to risk of RA and managing its symptoms. Smoking, physical activity, diet, and gut microbiota are considered to be the most essential modifiable factors in RA. Among dietary interventions, the most researched is Mediterranean diet, […]
- Comparative development of volatile-oriented multi-SPME and derivatisation-based GC×GC-TOFMS workflows for non-targeted faecal metabolomicson May 13, 2026
Gas chromatography-mass spectrometry (GC-MS) remains a key technique in metabolomics, yet most workflows rely on chemical derivatisation to enable the analysis of non-volatile metabolites. Although derivatisation broadens metabolite coverage, it increases sample preparation time and may introduce additional analytical variabilities. In contrast, solid-phase microextraction (SPME) enables rapid, solvent-free sampling of volatile and semi-volatile compounds, representing an attractive […]
Random Posts –
Featured Posts –
Latest from PubMed, #plant-based diet –
- Understanding preferences regarding protein-enriched plant-based products of patients with lived experience of (risk of) malnutrition – a grounded theory studyby Nathalie Gorter on May 14, 2026
CONCLUSION: Patients prefer varied, easy-to-eat plant-based products, avoiding strong smells, unhealthy ingredients, and large portions. Emphasizing shared values of health, sustainability, and animal welfare can promote adoption of plant-based options.
- Prediction of plant food allergens using protein embeddingsby Martín Méndez on May 14, 2026
MOTIVATION: The current trend to incorporate new protein sources to the diet, mostly from plants, requires a safety assessment of these polypeptides when used as food. Part of that safety evaluation involves assessing the potential allergenicity of the proteins. Such assessment typically follows a hierarchy of in silico, in vitro and in vivo assays. The computational prediction of protein allergenicity is the first step in the process and several predictors are available for this task. Due to…
- Meal-specific dietary patterns relate to memory functioningby Maria Kossowska-Wywiał on May 14, 2026
This research addresses a critical gap in our understanding of how specific meals consumed during the day relate to cognitive function, particularly memory performance. While numerous studies have explored overall dietary patterns, few have considered the isolated effects of specific meals. Across two studies, we investigated subjective and objective measures of memory in relation to dietary habits and meal-specific consumption among adults aged 20 to 90 years. In Study 1, individuals […]
- Gut microbiota-liver-kidney axis in diabetic kidney disease: mechanistic insights into amino acid metabolism and nutritional intervention strategies targeting natural bioactive compoundsby Li-Ya Sun on May 14, 2026
Diabetic kidney disease (DKD) is a leading cause of end-stage renal disease globally. Emerging research highlights the gut microbiota-gut-liver-kidney axis as a critical metabolic nexus linking dietary intake to DKD pathogenesis and progression. The gut microbiota, acting as a vast metabolic organ, transforms dietary components into key metabolites. Beneficial fermentation of fiber produces short-chain fatty acids (SCFAs) like butyrate, which exert anti-inflammatory and renal protective […]
- Plant-based diets for human health with implications for cardiometabolic health, gut microbiome, and nutritional adequacyby Mansour Alblaji on May 14, 2026
Plant-based diets have gained considerable interest in recent times due to their perceived health and environmental benefits. However, the term “plant-based diet” refers to a broad range of diets with a wide range of differences in food quality and nutritional content. This article aims to summarize the available evidence regarding the health and environmental impacts of plant-based diets, including new trends and issues. Epidemiological studies, RCTs, and life cycle assessment studies were…
- The zebrafish model: a versatile platform for uncovering the therapeutic potential of phytochemicals in liver diseasesby Yuliang Liu on May 14, 2026
The search for novel therapeutics for prevalent liver diseases such as metabolic dysfunction-associated steatotic liver disease, alcohol-related liver disease, and drug-induced liver injury is constrained by the methodological gaps in conventional preclinical models, which struggle to balance physiological complexity with screening efficiency. This challenge is particularly acute for natural products, where elucidating multifaceted mechanisms and inherent toxicological risks is paramount for…